Assessing the Effect of the Affordable Care Act on Part-Time Employment
The Patient Protection and Affordable Care Act of 2010, commonly known as the Affordable Care Act or ACA, requires larger employers to offer health insurance to their full-time workers or pay penalties for failing to do so. Under some circumstances, the law creates an incentive for employers to replace full-time labor with part-time labor. This Economic Brief considers recent research on whether the ACA has in fact increased the use of part-time labor.
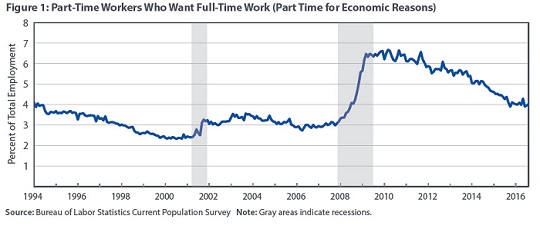
The percentage of American workers who are working part time for economic reasons (PTER) — that is, who would like to work full time but are unable to obtain full-time work — increased substantially during the 2007–09 recession. The percentage has remained elevated during the recovery. (See Figure 1 below.)
The ACA places requirements on employers with a sufficiently large workforce to offer health insurance to at least 95 percent of their U.S.-based full-time workers or pay sizable penalties.
Employers can avoid or minimize the costs associated with these requirements, however, by reducing their use of full-time employees. Strategies for doing so include automation of work currently performed by full-time employees; contracting out the tasks of full-time employees (although the employer still might bear some costs of the requirements if the contract firm also is subject to the requirements and is able to pass some of the associated costs back to the employer); and substituting part-time workers for full-time workers.
Through the incentive created by the ACA for employers to shift from full-time to part-time labor, it is possible that the legislation has influenced the elevated level of PTER. Based on anecdotal evidence of employers posting jobs with schedules up to twenty-nine hours per week — just below the ACA’s cutoff of thirty hours per week in its definition of full-time employment — some observers have suggested that this incentive is indeed leading to shifts in the labor market.1 Economic research has attempted to assess the extent, if any, to which the ACA has been having such an effect. But this research has been complicated by issues related to delays in the law’s implementation.
What Is “Part-Time” Employment?
The Bureau of Labor Statistics Current Population Survey (CPS) distinguishes several types of part-time employment. As noted, PTER, also known as involuntary part-time, consists of workers who would like to work full time but work part time. Within this category, the CPS distinguishes between those who report that they work part time because of slack work or adverse business conditions and those who report that they are unable to find full-time work. Part-time workers who do not wish to work full time — for example, on account of school, family obligations, or health limitations — are classified as part-time for non-economic reasons (PTN), also called voluntary part-time. The CPS defines “full-time” as thirty-five hours per week or more, in contrast with the ACA’s thirty hours per week and the colloquial understanding of forty hours per week.
Part-time work, both voluntary and involuntary, is more prevalent among younger workers. In addition, PTER is generally the most concentrated among less-educated workers and among workers in low- and medium-skill occupations.2
The ACA Employer Mandate
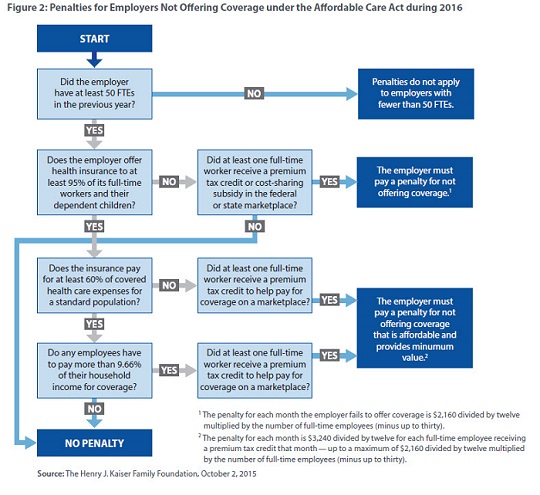
The ACA’s employer mandate applies to private firms, nonprofits, and governmental organizations employing at least fifty full-time-equivalent employees — that is, fifty full-time employees or an equivalent combination of full-time and part-time employees. An employer within this category is known as an “applicable large employer” and is required to offer health insurance to 95 percent of its full-time workers, including their children up to age twenty-six. (See Figure 2 below.) The plan must be “affordable,” meaning that its cost to the employee is no more than 9.66 percent of the employee’s household income.3 Because an employer typically does not know an employee’s household income, however, the law allows the employer to use a percentage of the employee’s pay, among other options, as an alternative basis for determining the employee’s maximum cost.
Depending on circumstances, the cost of the mandate for each full-time employee may be significant. ADP, a global human capital management firm, has estimated that in 2015, a large employer (one with 1,000 or more employees) faced, on average, annual premiums of $10,440 for each covered worker.4 (The actual premium for a given worker varies substantially with the number of dependents.) For highly paid employees, the premiums can be charged in full to the employee and still be “affordable” under the ACA’s definition. For lower-paid employees, however, the employer must absorb part of the cost to meet the requirement of affordability. For example, assuming an annual premium of $10,440, workers on a forty-hour-per-week schedule earning $20 per hour could be charged no more than $4,019 per year (9.66 percent of $41,600), yielding an employer subsidy of $6,421 each. An hourly wage of $15 with a thirty-hour-per-week schedule — considered full-time for purposes of the ACA — would entail a subsidy of $8,180, adding approximately 35 percent of the worker’s wages to the cost of his or her employment.
In theory, employers may be able to shift a larger portion of the insurance cost onto employees simply by reducing the workers’ hourly wages in lieu of explicitly charging them for insurance.5 But for some employees, minimum wage laws would limit an employer’s ability to do so. Moreover, employers historically have appeared reluctant to cut nominal wages, a phenomenon known as downward nominal wage rigidity, which may result from concerns about worker demoralization.
If an employer fails to offer the required coverage, penalties are assessed based on the number of full-time employees and the number of months an employer does not offer coverage. If an employer offers coverage, but it is not affordable with respect to some employees, penalties are assessed based on the number of full-time employees who receive a federal subsidy for the purchase of a policy on a health insurance exchange. The penalties for noncompliance may be less than the cost of compliance in some instances, but they are nonetheless substantial and are not deductible from income for business income tax purposes.
As noted above, given the central role played by the employer’s number of full-time employees in determining the insurance costs and the penalties, employers may be motivated to change the size and structure of their workforces, either shedding full-time employees outright (through automation or contracting out) or substituting part-time schedules for full-time ones. A simple case of the latter would be reducing the hours of a thirty-hour-per-week employee to twenty-nine hours, converting the worker from full time to part time for purposes of the ACA and potentially saving thousands of dollars in subsidies or penalties. Another scenario is hiring workers only for twenty-nine-hour schedules who previously would have been hired for forty-hour schedules — in the process, increasing PTER.
At the same time, employers may be constrained by the unwillingness of workers to accept a lesser number of hours, by inefficiencies arising from shorter schedules, and other factors. Thus, an empirical question remains: Is the ACA contributing to PTER?
Questions about Timing
One challenge for researchers looking at the ACA employer mandate is the timing of its implementation. In July 2013, the imposition of employer penalties was delayed until 2015; in February 2014, the imposition of fines on employers with less than 100 full-time employees was delayed until 2016, and the coverage requirement for larger firms was reduced from 95 percent to 70 percent for 2015 (but not for later years). These delays give rise to an issue of how to define, for research purposes, the period when employers would have started responding (if at all) with workforce changes. It is plausible, but not empirically established, that employers generally took full advantage of the delays. It is possible, moreover, that some waited even longer in the expectation of continued delays. In addition, certain other features of the ACA’s implementation contributed to, in effect, a gradual imposition of its requirements.6
The timing issue is of particular importance for research that does not test the effects of the ACA for each year separately, but rather tests only an overall “before” period and an overall “after” period. In such research, the selection of an effective date that is too early may lead to attenuation of the ACA’s influence.
Research on the Employer Mandate and Part-Time Work
One variable affecting employers’ behavior is the extent to which they are able to shift premium costs onto workers. One of the first studies of the employer mandate considered a stylized model in which all of those costs are borne by workers and investigated the extent to which workers would prefer more or fewer working hours, given the costs of the premiums and the implicit tax created by the subsidy structure for marketplace insurance policies. That paper, by Casey B. Mulligan of the University of Chicago, suggested that workers in various circumstances may either reduce or increase their working hours in response to those taxes.7 He argued that the incentives created by the ACA will shift workers from work schedules in the 30- to 35-hour range to work schedules just below thirty hours, making them part-time under the ACA’s definition. In particular, based on the stylized model, he predicted that the ACA will increase the number of those working in the 26- to 29-hour range by 4.6 percent but increase the number of those working part time according to the CPS definition, that is, less than thirty-five hours, only by 2.5 percent. Most of this shift is predicted to occur for women and unmarried household heads. Overall, he predicted that the ACA would reduce total employment and hours worked by 3 percent.
Other empirical work has focused on the responses of employers to the mandate, which ultimately determines the effect, if any, on PTER. Surveys taken of employers have yielded mixed evidence. A 2015 study by ADP looked at payroll data from approximately 75,000 client organizations with fifty or more employees; it compared the part-time vs. full-time structures of the companies during the third quarter of 2013 and the third quarter of 2014.8 The study found that in the aggregate, the percentages of employees on schedules of under 30 hours, 30 to 34 hours, and 35 or more hours showed little or no change between the two periods. In particular, the percentage of employees working less than 30 hours per week was 13.6 percent in the third quarter of 2013 and 13.3 percent in the third quarter of 2014, essentially no change. ADP found the same pattern when it broke down the data by industry.
A 2015 employer survey by the Kaiser Family Foundation of employers with fifty or more full-time-equivalent employees found that 4 percent of respondents reported they had changed some jobs from full-time to part-time in response to the mandate and that 4 percent of respondents reported that they had cut the number of full-time employees they planned to hire in response to the mandate.9 But 10 percent of employers reported changing some jobs from part-time to full-time so they would become eligible for benefits. (The study did not include data on the number of affected employees in each of these categories, and thus it reached no conclusion on the mandate’s net effect.)
A 2016 article in Applied Economics Letters by Aparna Mathur and Michael R. Strain of George Mason University and Sita Nataraj Slavov of the American Enterprise Institute looked at CPS data from January 2008 through July 2014, focusing on the relative employment size of those working 25 to 29 hours per week (just under the ACA’s definition of “full-time”) and 31 to 35 hours per week (just over the ACA’s definition), the adjustment margin emphasized by Mulligan.10 The authors compared the periods before and after March 2010, the month of the law’s passage and signing. They found that the enactment of the ACA was associated with a shift of workers from the 31 to 35 hour full-time group to the 25 to 29 hour part-time group. But several groups that they hypothesized would be affected more heavily by the mandate — those employed in the retail or hospitality industries; those working in buildings and grounds cleaning and maintenance, personal care and service, or food preparation and service; and those earning under $10 per hour — did not show a more pronounced shift than their overall sample. Consequently, they concluded that the ACA did not cause the shift from full-time to part-time.
In a 2015 working paper, William E. Even of Miami University and David A. Macpherson of Trinity University estimated the effects of the ACA in a two-step process.11 First, they estimated the fraction of workers potentially affected by the mandate (by virtue of their full-time status and lack of insurance coverage) for a baseline period, 2003–07. They did so on an industry-by-industry basis and at various education levels. Second, they estimated the likelihood of PTER employment for workers in the different industries, accounting for differences in demographic compositions across industries; they estimated these likelihoods for each year from 2010 through 2014. Finally, they analyzed whether the yearly changes in the likelihood of PTER across industries were related to the fraction of workers potentially affected by the ACA in those industries. They concluded that for workers without a college degree, the probability of increased PTER was highest in the industries with the highest shares of workers within the employer mandate. For college graduates, the relationship was statistically significant only for 2014.
Even and Macpherson also carried out a similar analysis using occupation-specific estimates of the shares of workers within the mandate, rather than industry-specific estimates. The results by occupation yielded still stronger evidence of the ACA mandate pushing up PTER.
Conclusion
Although a strong theoretical argument can be made that the ACA employer mandate should increase the use of employees on a schedule of twenty-nine hours per week or less, empirical research so far has not unambiguously confirmed this prediction. With the exception of one study, survey data and econometric work has not found a large and statistically significant relationship between the mandate and part-time work. This may be related to the fact that the program’s implementation date has been in flux. If the ACA indeed increases part-time work but the impact of the ACA has been increasing over time (because of gradual or delayed implementation), research that relies on the date of the law’s enactment as its operative date would underestimate the mandate’s effects. The study that has found a relationship between the ACA and PTER, Even and Macpherson (2015), indeed also found that the impact has been increasing over time, consistent with the gradual implementation of the ACA.
Andreas Hornstein is a senior advisor and David A. Price is senior editor in the Research Department of the Federal Reserve Bank of Richmond.
See, for example, Ben Casselman, “Yes, Some Companies Are Cutting Hours in Response to ‘Obamacare,’” FiveThirtyEight.com, January 13, 2015; and “ObamaCare and the ‘29ers,’” Wall Street Journal, February 22, 2013.
Regarding the prevalence of part-time work among demographic groups and the transitions between full-time employment, PTER, PTN, unemployment, and out-of-the-labor-force status, see Maria E. Canon, Marianna Kudlyak, Guannan Luo, and Marisa Reed, “Flows to and from Working Part Time for Economic Reasons and the Labor Market Aggregates during and after the 2007–09 Recession,![]() ” Economic Quarterly, Second Quarter 2014, vol. 100, no. 2, pp. 87–111.
” Economic Quarterly, Second Quarter 2014, vol. 100, no. 2, pp. 87–111.
The percentage was set at 9.5 percent by the ACA but has been adjusted administratively to 9.66 percent for 2016 and is expected to be adjusted administratively in future years.
ADP Research Institute, “ADP Annual Health Benefits Report: 2015 Benchmarks and Trends for Large Organizations,” 2015, p. 17.
William E. Even and David A. Macpherson, “The Affordable Care Act and the Growth of Involuntary Part-Time Employment,” IZA Discussion Paper No. 9324, September 2015, p. 4.
Until 2016, employers were permitted to reduce their ACA liabilities by offering minimal “skinny” plans that did not cover hospital stays. See Jay Hancock, “Obama Administration Disallows Plans without Hospital Coverage,” Kaiser Health News, February 23, 2015; and Avik Roy, “Employers Can Minimize Their Exposure to Obamacare’s Penalties by Offering Low-Cost ‘Skinny’ Coverage,” Forbes.com, May 21, 2013.
Casey B. Mulligan, “The Economics of Work Schedules under the New Hours and Employment Taxes,” National Bureau of Economic Research Working Paper No. 19936, February 2014.
ADP Research Institute, “The Affordable Care Act and Economics of the Part-Time Workforce: Measuring the Impact of the Affordable Care Act,” 2015.
Kaiser Family Foundation, “Employer Health Benefits: 2015 Summary of Findings,” 2015, p. 6.
Aparna Mathur, Sita Nataraj Slavov, and Michael R. Strain, “Has the Affordable Care Act Increased Part-Time Employment?” Applied Economics Letters, 2016, vol. 23, no. 3, pp. 222–225. A working paper version is available online.
Even and Macpherson (2015)
This article may be photocopied or reprinted in its entirety. Please credit the authors, source, and the Federal Reserve Bank of Richmond and include the italicized statement below.
Views expressed in this article are those of the authors and not necessarily those of the Federal Reserve Bank of Richmond or the Federal Reserve System.
Receive a notification when Economic Brief is posted online.