Does Social Distancing Explain Variation in COVID-19 Infection Rates? A Cross-Regional Analysis
Does compliance with social distancing mandates explain regional variation in COVID-19 infection rates? For example, Europe was hit hard by the pandemic early on, but infection rates have steadily decreased since April, even as European governments have relaxed lockdown measures and opened borders to travelers from other European countries. In contrast, the United States is experiencing a resurgence of daily cases driven by outbreaks in the south and west. Arizona, California, Florida, and Texas currently account for 50 percent of new daily cases in the United States. Both pundits and policymakers have pointed to a lack of social distancing to explain the differing trend in the United States. In this article, we study this hypothesis using mobility measures such as "time spent at home" or "time spent at retail" as an indicator of social distancing.
Regional Differences in Infection Rates and Deaths
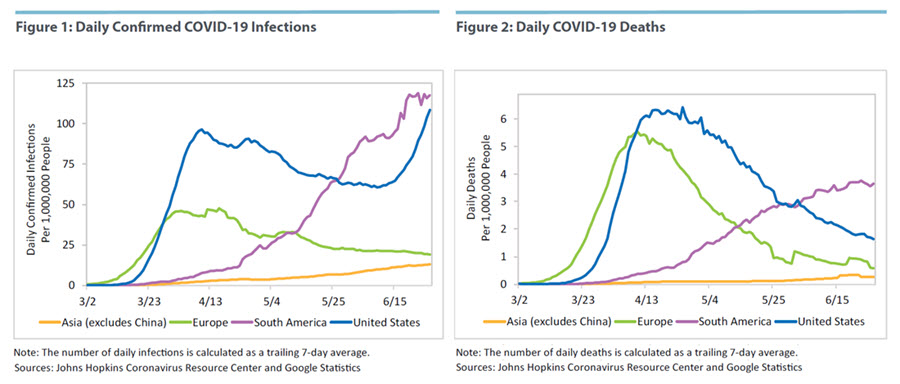
Using data from Johns Hopkins Coronavirus Resource Center and Google Statistics, Figures 1 and 2 present daily confirmed infections and daily deaths per 1,000,000 inhabitants for Asia (excluding China), Europe, South America, and the United States. (Countries included in the calculations are listed at the end of this article.) Europe and the United States follow a similar trajectory until early June. After that, daily confirmed infections in the United States rise sharply but continue to decline in Europe. (The U.S. death rate does not exhibit a similar increase in our sample. This could be because there is a lag of several weeks between infection and death or because the demographics of those infected has changed.) In any case, many are wondering about the United States' lack of containing the growth of daily infections. Were European governments' responses to the pandemic more efficient than the U.S. government's response? Did European citizens comply more with social distancing guidelines than U.S. citizens?
Regional differences are also apparent looking at Asia and South America. South America has been called the new epicenter of the epidemic, as many countries are seeing the daily count of both infections and deaths steadily increase. The total number of cases is around four times higher than the number in April. Many observers blame the deteriorating situation on the inadequate government response. Many governments played down the severity of the threat. For example, Brazil, the most populous country in the region, has given out guidelines but has not imposed national restrictions amid a major COVID-19 outbreak. On the flip side, however, Argentina and Colombia imposed strict social distancing measures, but daily infections still soared. Asia (excluding China) is also experiencing an increase, albeit much smaller than South America, driven by India and Pakistan. India enacted a lockdown measure early in March, but this measure did not prevent workers from fleeing cities and returning to their villages in crowded buses and trains. In Pakistan, the government eased the nationwide lockdown despite warnings from health experts.
Time Allocation Across Regions
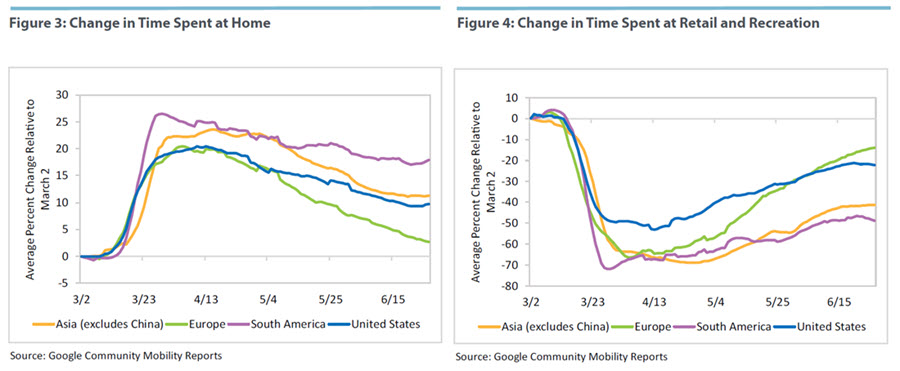
One way to study the connection between social distancing and infection rates is to use mobility measures as proxies for social distancing. To this end, we use data from the Community Mobility Reports by Google. The data are based on the location of users and are disaggregated by particular destinations: grocery and pharmacy, parks, transit stations, retail and recreation, residential (denoted as "home" in the figures below), and workplace.
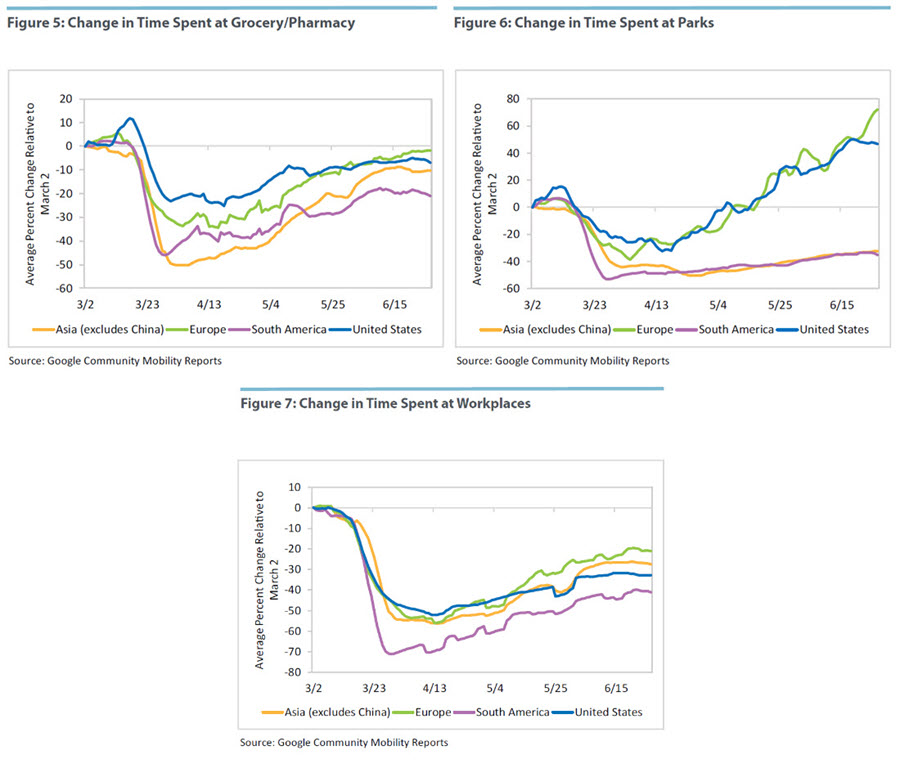
Figures 2-7 plot time series for the regional time allocation for five categories: time spent at home, time spent at retail and recreation, time spent at grocery and pharmacy, time spent at parks, and time spent at work. (Note that adding up all these categories does not necessarily exhaust the amount of available time in a day as some activities may not be documented, such as being outdoors but not in a location included in the categories Google follows). Although the United States, unlike Europe, has experienced a rise in confirmed infections during the past month, the overall U.S. mobility data do not show any significant divergence from past trends or relative to Europe. If anything, inhabitants of European countries have been reducing time spent at home at a faster rate than the U.S. population during the past month and have been increasing time spent at retail, groceries, and work at a faster rate. The main difference between the United States and Europe is in the overall level of the decrease in mobility. Visits to retail and grocery establishments declined substantially less in the United States than in Europe during the first months. But all measures have been converging as of June. Adding to the puzzle, both Asia and South America reduced their time outside home to a larger degree than Europe and the United States during the first couple of months of the pandemic, which seems to contradict the strong increase of daily infections observed in those regions. For example, in the average South American country, time spent at home is currently 20 percent higher than on March 2, while in the United States it is 10 percent higher, and in Europe it is just 5 percent higher.
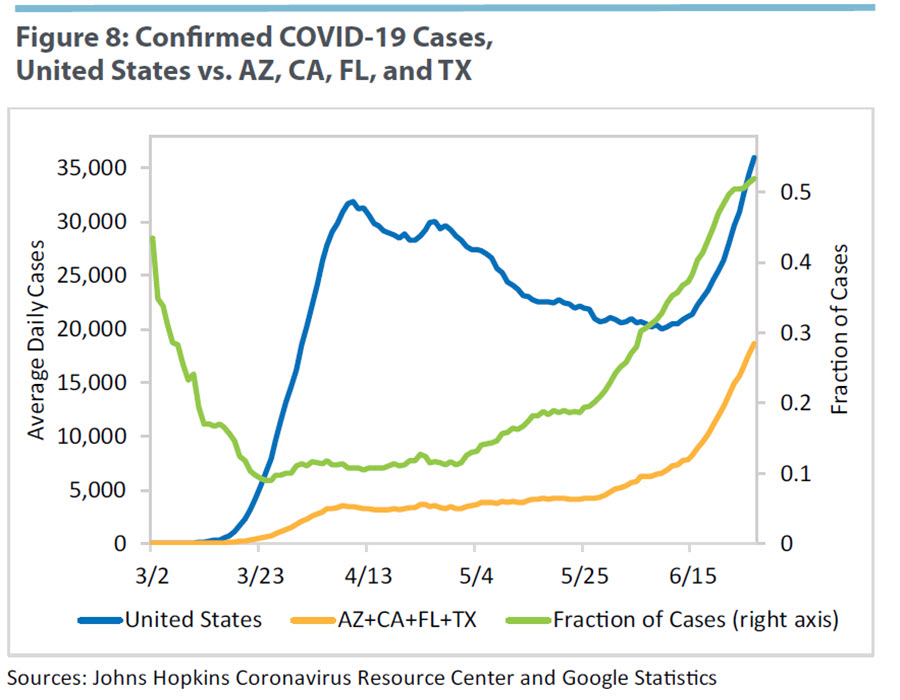
Thus, mobility patterns are, at most, weakly related to infection rates at the country level. But how about within the United States? Can we relate mobility measures to the recent surge of cases in Arizona, California, Florida, and Texas? Figure 8 confirms that the surge of U.S. infections stems from these states. Currently, around 50 percent of daily infections in the country are due to infections in Arizona, California, Florida, and Texas. At the end of May, these states accounted for around 20 percent of the overall cases, while they now account for more than half of new daily national cases.
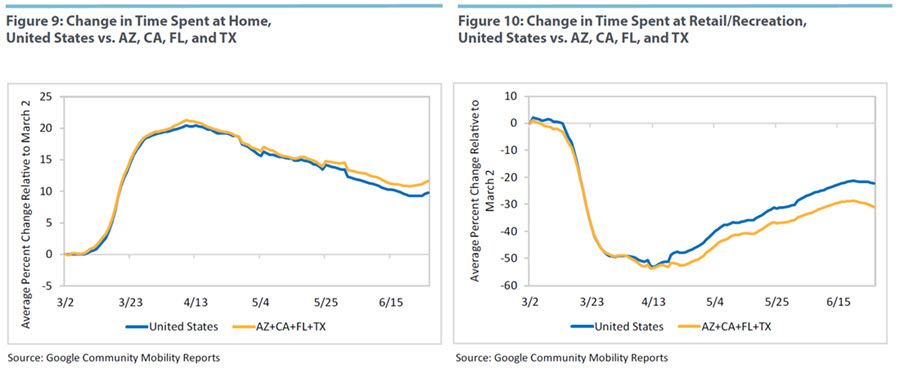
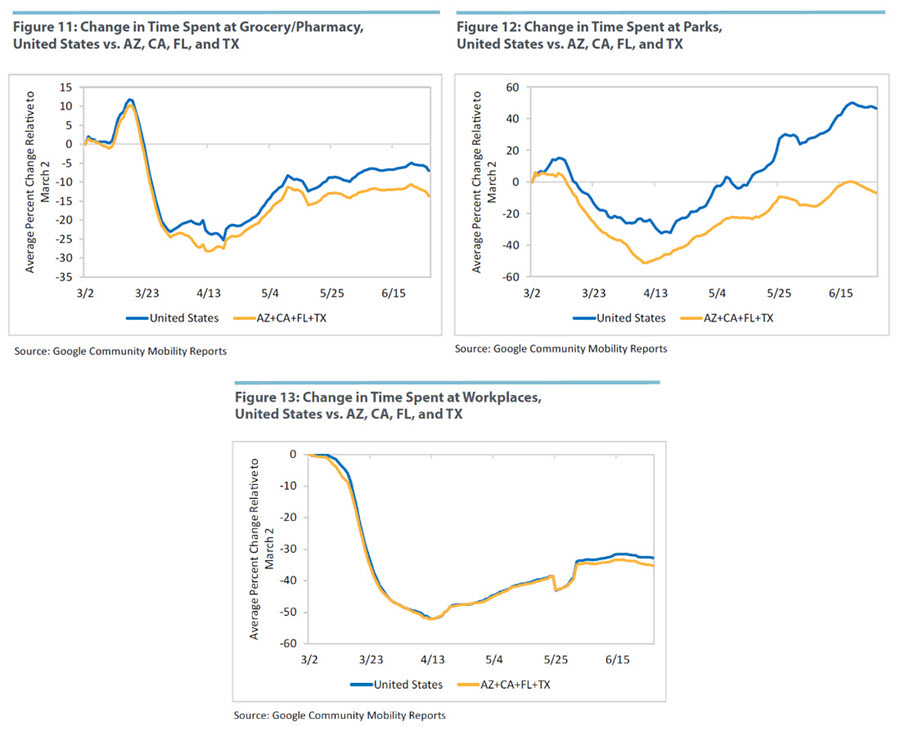
But once more, our mobility data do not indicate that residents in these four states spent more time outdoors than U.S. residents as a whole. As seen in Figures 9-13, the time spent at home is on the same decreasing trajectory as in the United States overall. Time spent at parks has not bounced back as fast, maybe due to landscape or weather in these states. And time spent at workplaces, retail and recreation, and grocery and pharmacy features broadly the same pattern as the country as a whole.
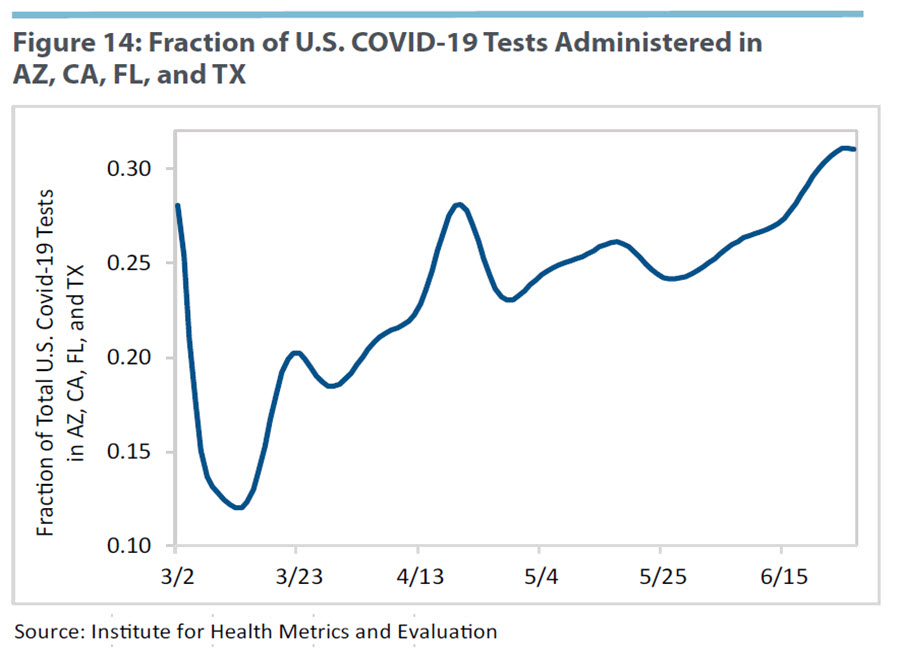
A potential explanation for the rise in cases in these states relative to the United States is the increase in the number of tests. For a given number of infected people, an increase in the share of tests in a location implies an increase in the share of confirmed infections of that location relative to the country. Figure 14 shows the share of daily total U.S. tests performed in Arizona, California, Florida, and Texas using data from the Institute for Health Metrics and Evaluation. This share increased 5 percentage points in June. But as seen in Figure 8, the share of daily confirmed cases in these states increased in June by 30 percentage points (from 20 percent to 50 percent). Therefore, the relative increase in testing cannot by itself account for the recent increase of daily infections in these four states.
Some Final Remarks
We have found that mobility measures are weakly related to the number of daily infections, both across regions at a global scale and across U.S. states, and that the increased number of tests seems to account for only a small part of the regional differences within the United States. Some additional remarks are in order. First, a broad, aggregated analysis of time allocation across regions does not take into account the ability to move within a region. For example, it is harder to travel without restrictions across subregions in Europe than it is in the United States. Although Europe and the United States are roughly of the same geographical size, Europe consists of numerous countries (36 in our sample) that are able to close their borders to travelers. This means that a European citizen can travel without restrictions within a land area 36 times smaller than a U.S. citizen. If traveling contributes to spreading the virus, the United States is in a far worse position than Europe.
Second, there is a distinction between the time spent outdoors and the effectiveness of social distancing. The ability to engage in effective social distancing outdoors often depends on the city structure (spacious versus crowded workplaces and shopping stores, reliance on public transportation, etc.), as well as residents' willingness to engage in preventive activities such as wearing face coverings in public spaces or maintaining physical distance from others. It would be interesting to quantify these channels in future work and estimate their impact on regional differences on infection rates.
Marios Karabarbounis is an economist, Matthew Murphy is a research associate, and Nicholas Trachter is a senior economist in the Research Department of the Federal Reserve Bank of Richmond.
List of Countries Included in Our Sample by Region
Asia: India, Indonesia, Pakistan, Bangladesh, Japan, Philippines, Vietnam, Turkey, Thailand, Myanmar (formerly Burma), South Korea, Iraq, Afghanistan, Saudi Arabia, Malaysia, Yemen, Nepal, Taiwan, Sri Lanka, Kazakhstan, Cambodia, Jordan, United Arab Emirates, Tajikistan, Israel, Hong Kong, Laos, Kyrgyzstan, Singapore, Oman, Kuwait, Georgia, Mongolia, Qatar, Bahrain
Europe: Russia, Germany, United Kingdom, France, Italy, Spain, Ukraine, Poland, Romania, Netherlands, Belgium, Czech Republic, Greece, Portugal, Sweden, Hungary, Belarus, Austria, Serbia, Switzerland, Bulgaria, Denmark, Finland, Slovakia, Norway, Ireland, Croatia, Moldova, Bosnia and Herzegovina, Estonia, Lithuania, North Macedonia, Slovenia, Latvia, Luxembourg, Malta
South America: Brazil, Colombia, Argentina, Peru, Venezuela, Chile, Ecuador, Bolivia, Paraguay, Uruguay
This article may be photocopied or reprinted in its entirety. Please credit the authors, source, and the Federal Reserve Bank of Richmond and include the italicized statement below.
Views expressed in this article are those of the authors and not necessarily those of the Federal Reserve Bank of Richmond or the Federal Reserve System.